Rotator Cuff Repair – Advanced Orthopedic Surgery for Shoulder Injuries
Overview of Rotator Cuff Repair
Rotator cuff repair is a surgical procedure to repair torn tendons in the shoulder. It helps restore shoulder movement and reduces pain. It is typically performed when non-surgical methods like physical therapy and medications have not provided relief.
Arthroscopic Technique for Rotator Cuff Repair
In rotator cuff repair surgery, small incisions are made around the shoulder to insert an arthroscope—a small camera—and specialized instruments. The surgeon trims the damaged tendon edges and reattaches the tendon securely to the bone using suture anchors. The procedure uses tools like shaver systems, RF cautery machines, sheaths, and surgical cameras for clear visualization and precise work. These instruments ensure minimal damage to surrounding tissue and enhance healing. The surgeon may choose between an open approach or a minimally invasive arthroscopic method. A sling or immobilizer is typically used post-surgery to protect the repair and support recovery.
Conditions Requiring Rotator Cuff Repair Surgery
- To repair a torn rotator cuff tendon causing persistent shoulder pain and weakness
- To improve shoulder function and mobility when conservative treatments fail
- To prevent further degeneration of the tendon and surrounding muscles
- To restore normal daily and athletic shoulder activities
- To reduce risk of future joint damage or degeneration due to instability
Surgical Instruments Used for Rotator Cuff Repair
- Arthroscopy Shaver System
- Arthroscopy RF Cautery Machine
- Arthroscopy Sheath
- Arthroscope (Camera System)
- HD Camera System
- Arthroscopy Suction Tube
- Arthroscopy Instrument Set (e.g., forceps, scissors, graspers)
- Arthroscopy Shaver Blades
- RF Probes / Electrodes (part of RF Cautery Machine system)
- Irrigation Pump (Arthro Pump)
Leading Countries Performing Rotator Cuff Repair
- United States
- Germany
- Japan
- United Kingdom
- Australia
Post-Surgery Improvements
- Restores muscular strength and joint stability in the shoulder
- Provides precise tendon reattachment with minimal tissue damage
- Promotes faster recovery and shorter rehabilitation time
- Reduces postoperative pain and risk of scar tissue formation
- Enhances long-term shoulder function and active lifestyle retention
Aomax Ortho is a leading manufacturer of rotator cuff repair-related instruments and implants, offering innovative, high-quality solutions trusted by orthopedic surgeons worldwide.
Get Connected:
+91 98989 50530 | exports@aomaxortho.com | www.aomaxortho.com
Meniscus Repair – Effective Orthopedic Procedure for Torn Knee Cartilage
Basics of Meniscus Repair / Meniscectomy
Meniscus repair and meniscectomy are surgical procedures used to treat tears in the knee’s meniscus, a cartilage that cushions the joint. Meniscus repair involves stitching the torn cartilage back together, while meniscectomy entails removing the damaged portion. These surgeries aim to alleviate pain and restore knee function, especially after injury or degeneration.
Surgical Approach and Techniques
Both procedures are typically performed arthroscopically, using small incisions and a camera to guide the surgery. In meniscus repair, the torn edges are sutured together, promoting healing, particularly in areas with good blood supply. Meniscectomy involves trimming or removing the damaged meniscal tissue to relieve symptoms. The choice between repair and meniscectomy depends on factors like the tear’s location, patient’s age, activity level, and overall knee health. While meniscectomy offers quicker symptom relief, meniscus repair is preferred when feasible, as it preserves the cartilage and reduces long-term arthritis risk. Recovery times vary, with meniscus repair generally requiring a longer rehabilitation period.
Purpose of the Surgery
- To treat meniscus tears resulting from sports injuries, trauma, or degenerative changes.
- To alleviate knee pain, swelling, and instability caused by meniscal damage.
- To restore knee function, enabling patients to return to daily activities and sports.
- To prevent further joint damage and reduce the risk of developing osteoarthritis.
Equipment and Tools Used For Meniscus Repair / Meniscectomy
- Arthroscope
- Meniscal repair sutures
- Shaver blades
- Graspers
- Cannulas
- Meniscal anchors
- Radiofrequency probes
- Surgical scissors
- Fluid management systems
- Arthroscopic pumps
Top 5 Countries of Meniscus Repair / Meniscectomy
- United States
- Germany
- Japan
- South Korea
- United Kingdom
Benefits and Impact of Meniscus Repair / Meniscectomy
- Preserves knee joint function by repairing or removing damaged tissue.
- Reduces pain and inflammation effectively.
- Speeds up recovery compared to open surgery methods.
- Minimizes damage to surrounding healthy cartilage.
- Helps prevent early onset of knee arthritis.
Aomax Ortho is a leading manufacturer of meniscus repair and meniscectomy related products, providing high-quality surgical instruments and materials for orthopedic procedures.
Get Connected:
+91 98989 50530 | exports@aomaxortho.com | www.aomaxortho.com
ACL Reconstruction Surgery – Precision Care for Anterior Cruciate Ligament Injuries
ACL Reconstruction Introduction
ACL Reconstruction is a surgical procedure to fix a torn anterior cruciate ligament in the knee. This ligament is important for keeping the knee stable, especially during movement. The surgery involves replacing the damaged ligament with a graft taken from another part of the body or a donor.
Surgical Procedure of ACL Reconstruction
During ACL reconstruction, the surgeon first makes small cuts around the knee to insert a tiny camera and surgical instruments. The torn ACL is removed, and a new graft—usually from the patient’s hamstring, patellar tendon, or a donor—is carefully placed. This graft acts like a new ligament to support knee movement. Special surgical drills and arthroscopic tools are used to create tunnels in the bones to secure the graft. Screws or other fixation devices are then used to hold the graft in place until it heals. The surgery is minimally invasive and helps restore full knee function over time.
Why Doctors Recommend ACL Reconstruction
- To treat a complete ACL tear that causes knee instability.
- To help athletes or active individuals return to sports or physical activities.
- To prevent further damage to the knee joint, including cartilage or meniscus injury.
- When physical therapy fails to improve symptoms or function.
Instrumentation & Products for ACL Reconstruction
- ACL PCL Instrument Set: Specialized set for graft preparation, drilling, and fixation in cruciate ligament surgeries.
- Arthroscopy Shaver System and Shaver Blade: For debridement, shaping, and cleaning joint tissues during minimally invasive procedures.
- RF Cautery Machine: Provides precise cutting and coagulation under arthroscopic conditions.
- Arthroscope, Camera System, Sheath, Forceps, Graspers, and Suction Tubes: Essential for visualizing and maneuvering within the joint.
- Interference Screws (e.g., stainless steel or PEEK) for graft fixation.
- Endo-Button devices (Continuous Loop, Flexible Loop, Fixed Loop, with washer, etc.) to secure grafts effectively.
- Low-Profile Cancellous Screws, Titanium Washers, Ligament Staples—used to reinforce graft fixation and ensure stability.
Top Nations in ACL Reconstruction Surgery
- United States
- Germany
- Japan
- South Korea
- Australia
Key Benefits of Undergoing ACL Reconstruction
- Improves knee stability and prevents the joint from giving out.
- Restores strength and full range of motion to the knee.
- Reduces long-term risk of osteoarthritis after an ACL injury.
- Allows safe return to sports or physical activities.
- Minimally invasive techniques lead to faster recovery and less scarring.
Aomax Ortho is a leading global manufacturer of ACL Reconstruction-related instruments and implants, offering precision-engineered tools trusted by orthopedic surgeons for advanced ligament repair.
Get Connected:
+91 98989 50530 | exports@aomaxortho.com | www.aomaxortho.com
PCL Reconstruction – Effective Orthopedic Procedure for Ligament Injuries
Overview of PCL Reconstruction Surgery
PCL Reconstruction is a surgical procedure to repair both injured posterior cruciate ligaments in the knee. This surgery is typically done after severe trauma or sports injuries that affect both PCL bundles. It helps restore knee stability and improve mobility.
The Surgical Technique Behind PCL Reconstruction
In this procedure, surgeons reconstruct both the anterolateral and posteromedial bundles of the PCL using tendon grafts. The surgery is performed using arthroscopy, a minimally invasive technique that involves a small camera and instruments inserted through tiny incisions. Hamstring tendons or allografts are commonly used to replace the damaged ligaments. Surgeons drill tunnels in the femur and tibia to position and secure the grafts with screws or buttons. Fluoroscopy and tensioning devices are often used for accurate placement and alignment. This advanced reconstruction improves knee function and prevents long-term joint instability.
When is PCL Reconstruction Necessary?
- To treat complete PCL ruptures involving both bundles.
- When conservative treatment fails to restore knee stability.
- In cases of multiligament knee injuries or high-grade posterior laxity.
- To prevent early-onset arthritis due to chronic PCL deficiency.
Essential Instruments and Implants for PCL Reconstruction
- Arthroscopic Camera System
- PCL Reconstruction Instrument Set
- Interference Screws
- Tibial Guide for PCL
- Femoral Aimer
- Graft Tensioner
- Soft Tissue Graft (Hamstring/Allograft)
- Suture Passer
- Cannulas for Arthroscopy
- Bioabsorbable Fixation Devices
Global Leaders in Double PCL Reconstruction
- United States
- Germany
- South Korea
- Japan
- India
Benefits of Double Bundle PCL Surgery
- Restores full knee stability after dual PCL injury.
- Improves joint biomechanics and functional movement.
- Reduces the risk of future meniscus or cartilage damage.
- Helps athletes and active individuals return to sports safely.
- Prevents chronic pain and long-term knee degeneration.
Aomax Ortho is a leading manufacturer of PCL Reconstruction related products, offering high-quality surgical tools and implants for orthopedic professionals worldwide.
Get Connected:
+91 98989 50530 | exports@aomaxortho.com | www.aomaxortho.com
Proximal Femoral Nail – Advanced Orthopedic Surgery for Hip and Femur Fractures
Basic Insight into the Procedure
Proximal femoral nail surgery is a procedure used to treat fractures of the upper femur near the hip. A long metal rod (nail) is inserted into the thigh bone to align and stabilize the broken segments. This helps the bone heal correctly and enables the patient to start moving sooner.
Nailing the Femur with Care: Surgical Process and Tools
During proximal femoral nail surgery, the patient is placed under anesthesia, and a small incision is made near the hip. The surgeon guides a wire down the center of the femur using real-time imaging (fluoroscopy), then drills and reams the canal to accommodate the intramedullary nail. The nail is inserted and secured with locking screws at both proximal and distal ends to ensure stability. Specialized instruments—like guide wires, reamers, targeting devices, and fluoroscopy equipment—help achieve accurate placement. The procedure promotes stable fixation and allows early weight-bearing.
When and Why This Surgery is Needed
- To treat inter- or pertrochanteric femoral fractures.
- For unstable subtrochanteric fractures requiring strong internal support.
- To manage fractures in osteoporotic or elderly patients.
- To enable early mobilization and reduce complications from immobility.
Essential Equipment for Proximal Femoral Nail Surgery
- Locking Profile Cancellous Screw (for stable fixation in spongy bone).
- Orthopaedic Probe (for tissue and bone exploration).
- Orthopedic Curette (for debridement at fracture site).
- Regular (Titanium) Washer (for load distribution under screws).
- Orthopedic Puncture Needle (for guiding or aspiration near bone).
- Arthroscopy Instruments Set – e.g., graspers and punch forceps (used in fracture assessment or minimally invasive visualization).
- Arthroscopy Shaver System or Blade (to clear debris or cartilage during evaluation).
- Arthroscopy Sheath (for maintaining clear visual access if arthroscopy is used adjunctively).
- Orthopedic Meniscotome (rarely, but potentially used in arthroscopic joint evaluation).
(Note: While not specific PFN nails, these instruments and fixation hardware are integral in proximal femoral nailing procedures.)
Top 5 Countries Performing Proximal Femoral Nail Surgery (most to least)
- India
- United States
- Germany
- Japan
- United Kingdom
Clinical Outcomes and Benefits
- Enables strong internal support, reducing risk of fracture displacement.
- Promotes early weight-bearing and shorter recovery time.
- Minimally invasive approach preserves soft tissue and blood supply.
- Lowers complication rates (e.g., infection, fixation failure) compared to open methods.
- Supports accurate anatomical alignment through guided instrumentation.
Aomax Ortho is a leading manufacturer of Proximal Femoral Nail Surgery-related products, offering high-quality fixation hardware and surgical instruments that support reliable and precise orthopedic trauma care.
Get Connected:
+91 98989 50530 | exports@aomaxortho.com | www.aomaxortho.com
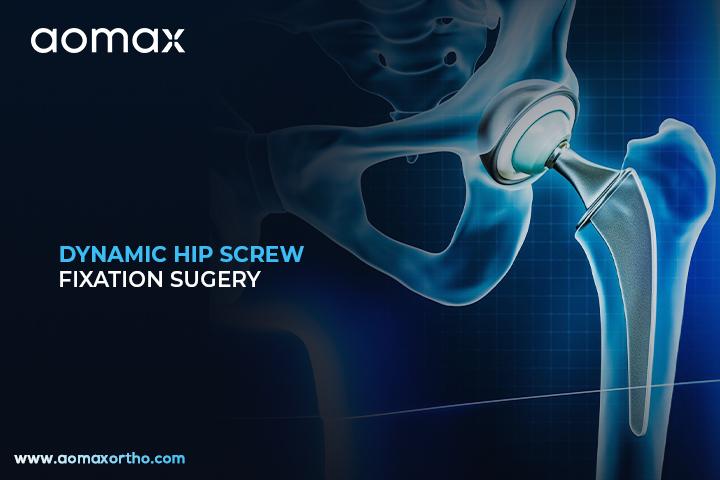
Dynamic Hip Screw Fixation – Precision Orthopedic Procedure for Fracture Stabilization
Understanding Dynamic Hip Screw (DHS) Surgery
Dynamic Hip Screw (DHS) Fixation is a surgical procedure used to treat specific types of hip fractures, particularly in older adults. The surgery involves inserting a large screw into the head of the femur (thigh bone) and attaching a side plate to the femoral shaft to stabilize the fracture. This method allows controlled movement of the femoral head, promoting healing and reducing complications.
Procedure Details of DHS Fixation
The DHS procedure begins with a small incision near the hip, through which the surgeon accesses the fractured femur. Using fluoroscopic imaging, a lag screw is precisely inserted into the femoral head, and a side plate is secured along the femoral shaft with multiple screws. This setup permits controlled sliding of the femoral head, facilitating compression at the fracture site, which is essential for healing. The design of the DHS allows for dynamic compression, enabling the bone to heal under the natural stress of weight-bearing activities. This technique is particularly beneficial for patients with osteoporotic bone, as it provides stability and promotes bone healing.
Medical Reasons for DHS Surgery
- To stabilize intertrochanteric and certain femoral neck fractures.
- To allow early weight-bearing and movement after hip fractures.
- To reduce pain caused by unstable fractures.
- To prevent complications such as bone misalignment or delayed healing.
Instruments and Implants Used in DHS Surgery
- Dynamic hip screw plate
- Large lag screw
- Cortical bone screws
- Guide wires
- Drill bits
- Targeting device (jig)
- Bone reduction clamps
- Surgical power drill
- Sterile surgical gloves
- X-ray imaging system (C-arm fluoroscopy)
Countries with Highest DHS Surgery Volume
- United States
- Germany
- United Kingdom
- India
- Japan
Benefits of Choosing DHS Surgery
- Promotes stable fracture healing with controlled compression.
- Enables early mobilization, reducing risk of complications from immobility.
- Minimally invasive compared to other fixation methods.
- Provides strong mechanical support for weight-bearing.
- Reduces hospital stay and improves functional recovery.
Aomax Ortho is a leading manufacturer of Dynamic Hip Screw (DHS) Fixation related products.
Get Connected:
+91 98989 50530 | exports@aomaxortho.com | www.aomaxortho.com
Minimally Invasive Plate Osteosynthesis – Effective Bone Stabilization with Less Trauma
Overview of Minimally Invasive Plate Osteosynthesis
Minimally Invasive Plate Osteosynthesis (MIPO) is a surgical technique used to stabilize fractures with minimal disruption to surrounding tissues. It involves inserting metal plates through small incisions to hold broken bones in place. This method promotes faster healing and reduces the risk of complications compared to traditional open surgery.
The MIPO Procedure Explained
MIPO is performed by making small incisions near the fracture site, allowing surgeons to insert plates without fully exposing the bone. Specialized imaging tools, such as fluoroscopy, guide the precise placement of these plates. The plates, typically made of titanium or stainless steel, are secured with screws to stabilize the fracture. This technique preserves the blood supply to the bone and surrounding tissues, which is crucial for healing. MIPO is particularly beneficial for fractures in areas with limited access or complex anatomy, as it reduces soft tissue damage and scarring.
When is MIPO Needed?
- To treat fractures with minimal soft tissue disruption.
- When traditional open surgery poses higher risks of infection.
- To preserve blood supply to the bone, aiding in faster healing.
- For fractures in complex or hard-to-reach areas.
Key Products Used in MIPO Surgery
- Locking Compression Plates (LCP)
- Titanium Bone Plates
- Low-Profile Cortical Screws
- Cannulated Screws
- Fluoroscopy Imaging Systems
- Bone Reduction Forceps
- Drill Guides for Minimally Invasive Surgery
- Screwdrivers with Minimally Invasive Tips
- Bone Clamps
- Surgical Retractors for Small Incisions
MIPO Surgery – Top Performing Nations
- United States
- Germany
- Japan
- South Korea
- France
Why Choose MIPO?
- Reduces soft tissue damage and scarring.
- Lowers the risk of infection due to smaller incisions.
- Maintains blood flow around the fracture, promoting faster healing.
- Enables earlier mobilization and rehabilitation.
- Minimizes postoperative pain and hospital stay.
Aomax Ortho is a leading manufacturer of Minimally Invasive Plate Osteosynthesis (MIPO) related products, offering high-quality plates and instruments designed to support effective fracture treatment.
Get Connected:
+91 98989 50530 | exports@aomaxortho.com | www.aomaxortho.com
Intramedullary Nailing – Precision Orthopedic Procedure for Fracture Fixation
Overview of Intramedullary Nailing
Intramedullary nailing is a surgical technique used to treat fractures of long bones such as the femur, tibia, or humerus. A sturdy metal rod is placed inside the bone’s central canal to align and stabilize the broken bone. This method helps healing and allows early movement in many cases.
How Intramedullary Nailing Is Performed and Supported by Surgical Tools?
The procedure is done under general or regional anesthesia using fluoroscopic X-ray guidance to ensure correct alignment. The surgeon begins by inserting a guidewire through a small incision into the marrow canal of the fractured bone. If needed, surgeons use reamers to enlarge the canal before inserting the nail. Once the nail is placed, locking screws are inserted proximally and distally to fix it securely. Instruments like insertion handles, targeting devices, reamers, guidewires, drills, and locking screws are essential throughout the operation. This stabilizes the bone internally and minimizes soft tissue damage, promoting faster recovery.
Clinical Indications
- To stabilize diaphyseal fractures of long bones (e.g., femur, tibia, humerus)
- In complex fractures such as comminuted, segmental, or displaced injuries
- For fractures due to osteoporosis or pathological conditions
- When non-surgical treatment fails or is impractical for healing
- To allow early weight-bearing and mobility, especially in lower limbs
Implants and Instruments Used
- Intramedullary Nails (femoral, tibial, humeral types)
- Locking Screws / Bolts
- Guidewires (ball-tipped or cannulated)
- Canal Reamers
- Insertion Handle / Nail Driver
- Targeting (Aiming) Device
- Cannulated Drill Bits
- Bone Tap Instruments
- Nail Extraction Tools
- Reduction Aids (e.g. percutaneous joysticks, Schanz screws)
Global Leaders in This Surgery
- United States
- Germany
- India
- China
- Brazil
Why Surgeons Prefer This Method
- High mechanical stability across fracture site
- Minimal soft tissue disruption and preservation of blood supply
- Strong axial, rotational, and length stability via locked fixation
- Enables early mobilization and shorter hospital stays
- Reduced risk of nonunion or malalignment
- Lower infection risk compared with external fixation
- Supports faster functional recovery and physical rehabilitation
Aomax Ortho is a leading manufacturer and exporter of orthopedic implants and instruments, including stainless steel and titanium products designed for surgeries like intramedullary nailing. Aomax is committed to global quality standards (ISO, CE, WHO-GMP) and serves partners in over 85 countries, with its manufacturing units based in Ahmedabad, Gujarat, India
Get Connected:
+91 98989 50530 | exports@aomaxortho.com | www.aomaxortho.com
External Fixation Surgery – Effective Treatment for Severe Bone Injuries
Introduction to External Bone Fixation
External fixation is a surgical method used to stabilize broken bones using a frame outside the body. The frame is connected to the bone through pins or wires inserted through the skin. This technique helps keep the bone aligned while it heals.
The Surgical Process Explained
The surgeon starts by inserting stainless steel or titanium pins or wires into the bone fragments through small incisions in the skin. These are connected to an external frame made of carbon fiber or stainless steel and fixed using clamps and connecting rods. Power drills, drill sleeves, coupling clamps, and tensioning devices are used during construction to ensure rigidity. The frame may be adjusted during healing to correct bone length or rotational alignment. Instruments such as external fixation frames, Schanz screws, connecting rods, clamps, and tensioning devices, support precise construction. This method is especially helpful when surrounding soft tissues are too fragile for internal fixation.
Indications for This Procedure
- Treatment of severe open fractures where the risk of infection is high
- Management of complex, unstable limb fractures requiring external support
- Bone lengthening or deformity correction procedures
- Temporary stabilization in polytrauma cases before definitive surgery
- Preservation of soft tissues when internal implants are contraindicated
Instruments Required
- External Fixator Frame
- Schanz Screws
- Connecting Rods
- Clamps for External Fixator
- Carbon Fiber Rods
- Pin-to-Rod Coupling Clamps
- Drill Sleeves
- Tensioning Devices
- Bone Drilling Machine
- Wire Fixation Bolts
Where External Fixation Is Most Common
- United States
- Germany
- India
- China
- Brazil
Key Advantages of External Fixation
- Allows stabilization of bone while preserving and protecting surrounding soft tissues
- Enables wound access and dressing changes without disturbing the fracture alignment
- Reduces risk of deep infection in contaminated or open fractures
- Permits gradual adjustment of bone alignment during recovery
- Supports correction of limb length discrepancies or bone deformities
- Provides rapid stabilization in emergency trauma scenarios
Aomax Ortho is a leading manufacturer of External Fixation related products, offering high-quality surgical tools such as frames, screws, rods, and tensioning devices that meet international standards and support orthopedic care globally
Get Connected:
+91 98989 50530 | exports@aomaxortho.com | www.aomaxortho.com
Closed Reduction and Internal Fixation – Advanced Technique in Orthopedic Trauma Care
CRIF – A Basic Surgical Outline
Closed Reduction and Internal Fixation (CRIF) is a method to fix broken bones without large surgical incisions. The surgeon first realigns the bone without opening the skin, then internal devices like screws or nails are inserted to stabilize it. CRIF helps bones heal accurately while minimizing trauma.
How CRIF is Performed?
Closed Reduction and Internal Fixation is performed using imaging tools such as fluoroscopy to guide the realignment of fractures. Once properly aligned, surgeons insert internal implants—such as screws, plates, or intramedullary nails—to maintain stable bone positioning. Specialized orthopedic instruments, often made of stainless steel or titanium, are used to place and secure these devices. The process uses small skin entries rather than a full open incision, preserving surrounding tissue. Advanced tools like cannulated screws and locking plates are standard for effective fixation. This combination promotes accurate healing and quicker return to function.
When is CRIF Needed?
- To treat displaced fractures where the bone is misaligned but soft tissue and skin remain intact.
- For complex or unstable fractures that require precise stabilization.
- To reduce surgical trauma and lower infection risk through minimal tissue dissection.
- To support faster recovery and enable earlier mobility, especially in active or elderly patients.
Surgical Tools and Implants Used in CRIF
- Bone Plates (e.g., dynamic compression and locking plates)
- Bone Screws (cancellous, cortical, cannulated screws)
- Locking Plates
- Locking Screws
- Interlocking Nails (e.g. proximal femoral nails)
- Kirschner Wires (K-Wires) and guide wires
- External Fixator Instruments (initial stabilization sets)
- Trauma Instrument Set (forceps, clamps)
- External Fixation Instrument Set
- Orthopedic Power Drill & Nail Instrument Set
Countries with Highest CRIF Volumes
- United States
- Germany
- India
- Japan
- Brazil
Surgical Outcomes and Benefits of CRIF
- Minimally invasive approach preserves soft tissues and reduces blood loss.
- Internal fixation provides strong stability, allowing accurate bone alignment and union.
- Lower infection rates compared to open surgeries due to small entry points.
- Enhanced precision using fluoroscopic guidance and modern implant design.
- Enables early weight-bearing or motion, speeding rehabilitation and reducing complications.
Aomax Ortho is a leading manufacturer of Closed Reduction and Internal Fixation related instruments and implants, offering high-quality stainless steel and titanium products trusted by orthopedic surgeons worldwide
Get Connected:
+91 98989 50530 | exports@aomaxortho.com | www.aomaxortho.com